Suksesvolle vertering begin by die kouproses in die mond gemeng met genoegsame speeksel.
Pierre-Ecohealth Blog Posts
Eco Health, Pet Health, Natural Health Products
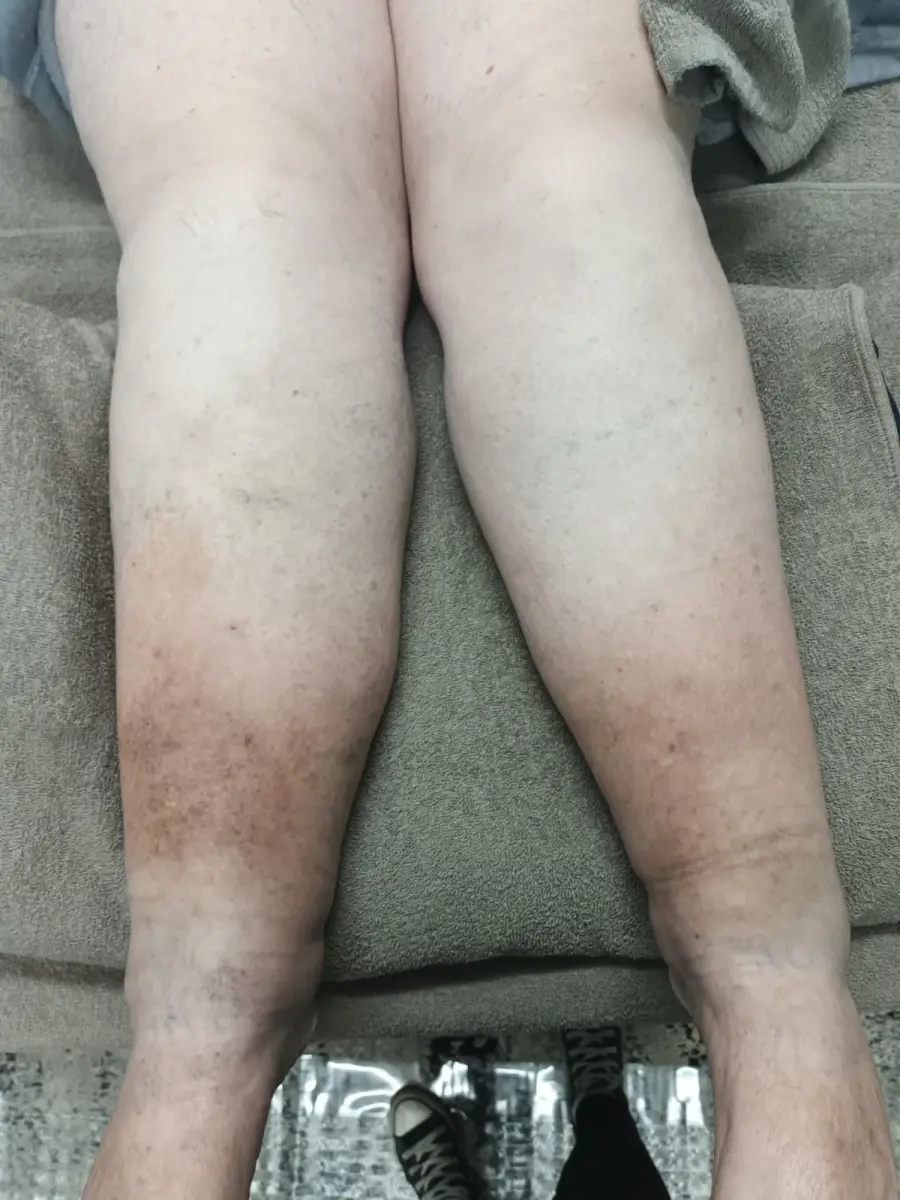
Agtergrond Amanda het geweldig gesukkel met swak bloedsomloop en waterretensie. Haar knieë was baie geswel van die vog en haar enkels en kuite was pers en vol seertjies van die swak bloedsirkulasie. Die linker knie was 2cm meer geswel as die regter knie, en die regterbeen se verkleuring was baie erger as die linker been. …
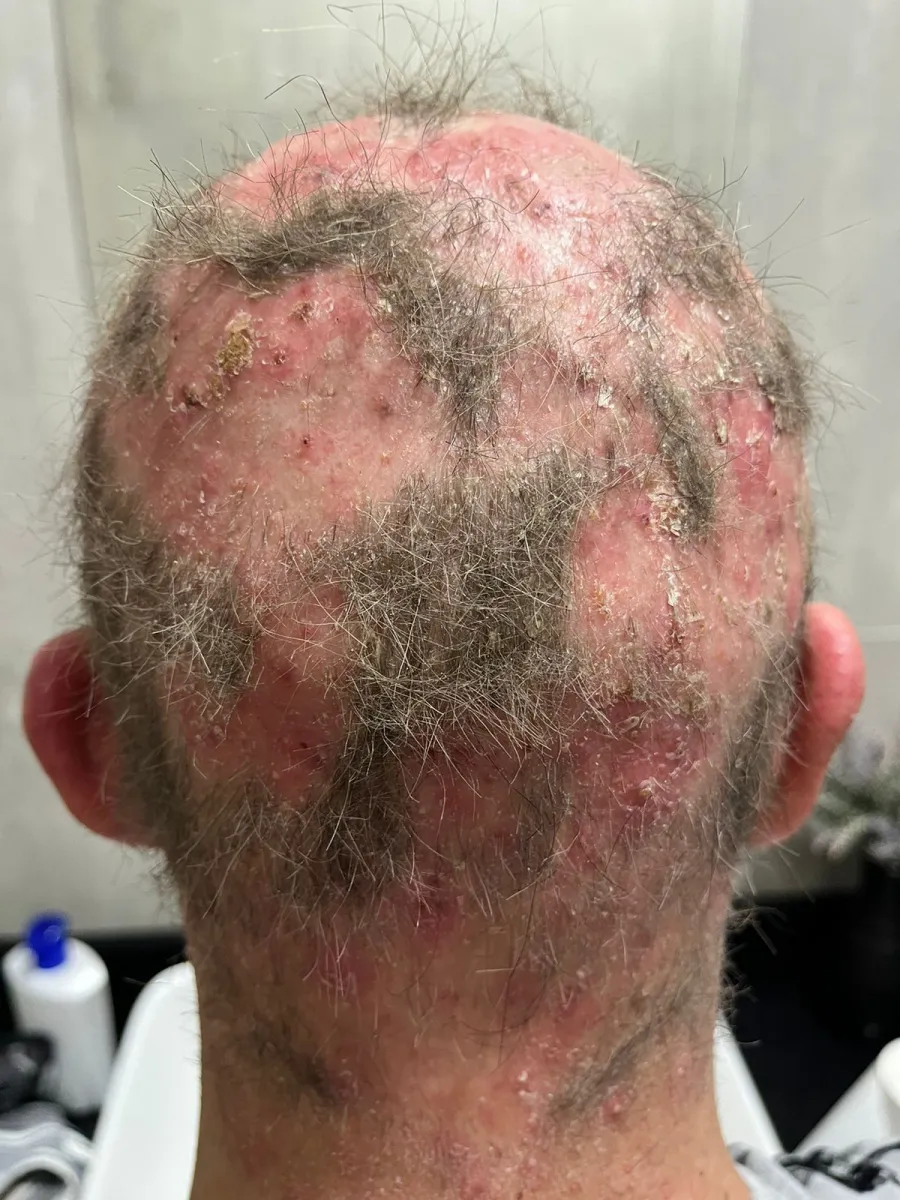
Skin care is a critical component in men and women. Here is what natural products did when there was no hope anywhere
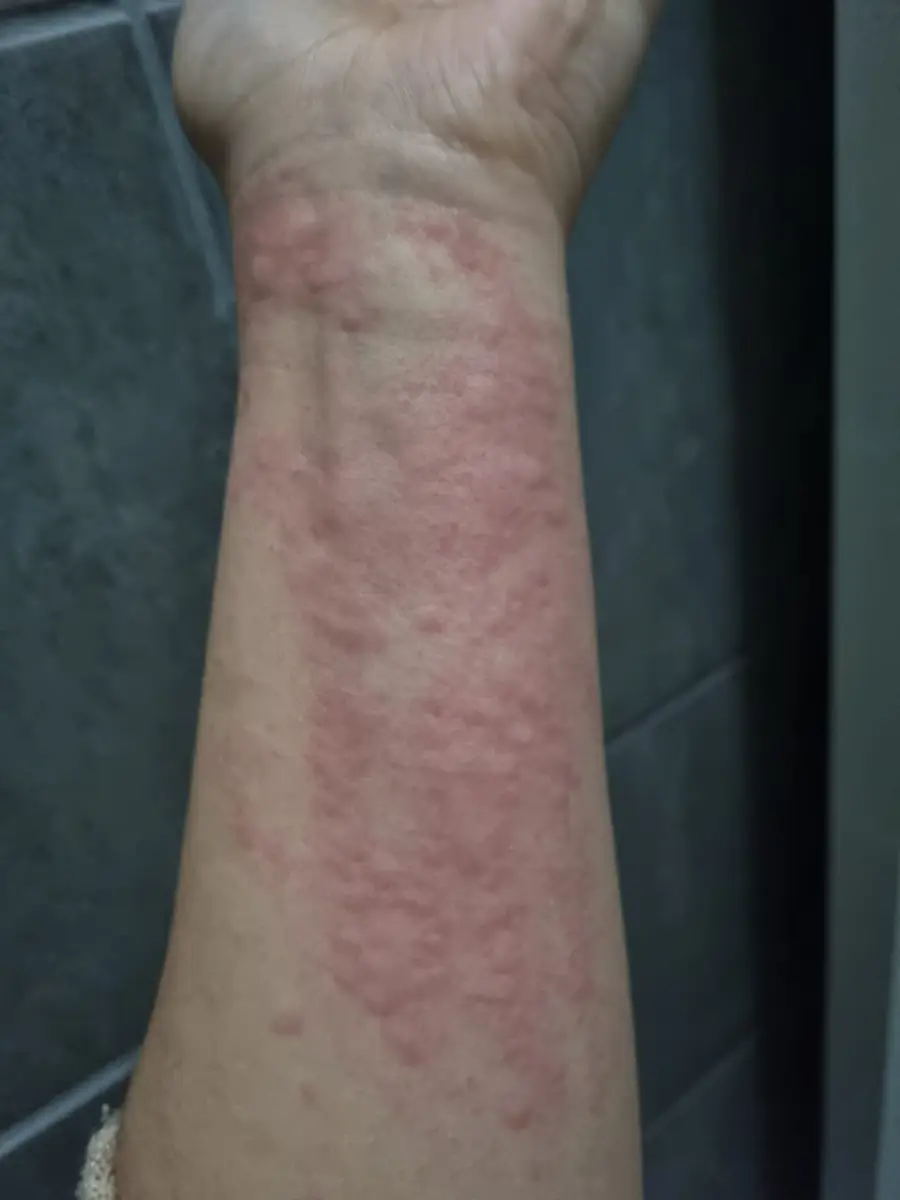
Desember 2021 het my vel-uitslag begin. Eers op my bene, toe na ‘n paar weke het dit versprei na my hele lyf. Na vele dokters En ‘n oordosis Allergex, Texa en Kortisoon (wat gif is vir enige diabeet) per dag, is ek verwys na die “Allergy Clinic”. Toetse is gedoen en ek is gediagnoseer met …
“The Department of Urology at Johns Hopkins Medical Institutions makes it clear that NO is the “main vasoactive nonadrenergic, noncholinergic neurotransmitter and chemical mediator of penile erection.
Impaired Nitric Oxide bioactivity is a major pathogenic mechanism of erectile dysfunction.”
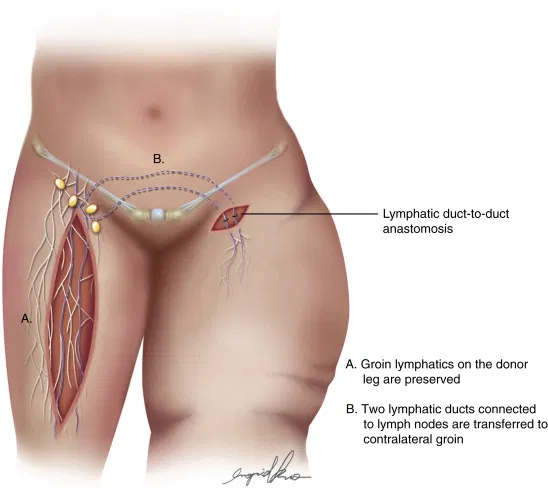
Die doel van ‘n persoon se limfvatstelsel, naas belangrike immuunfunksies, moet dien as die tweede “riool” of dreineringstelsel.
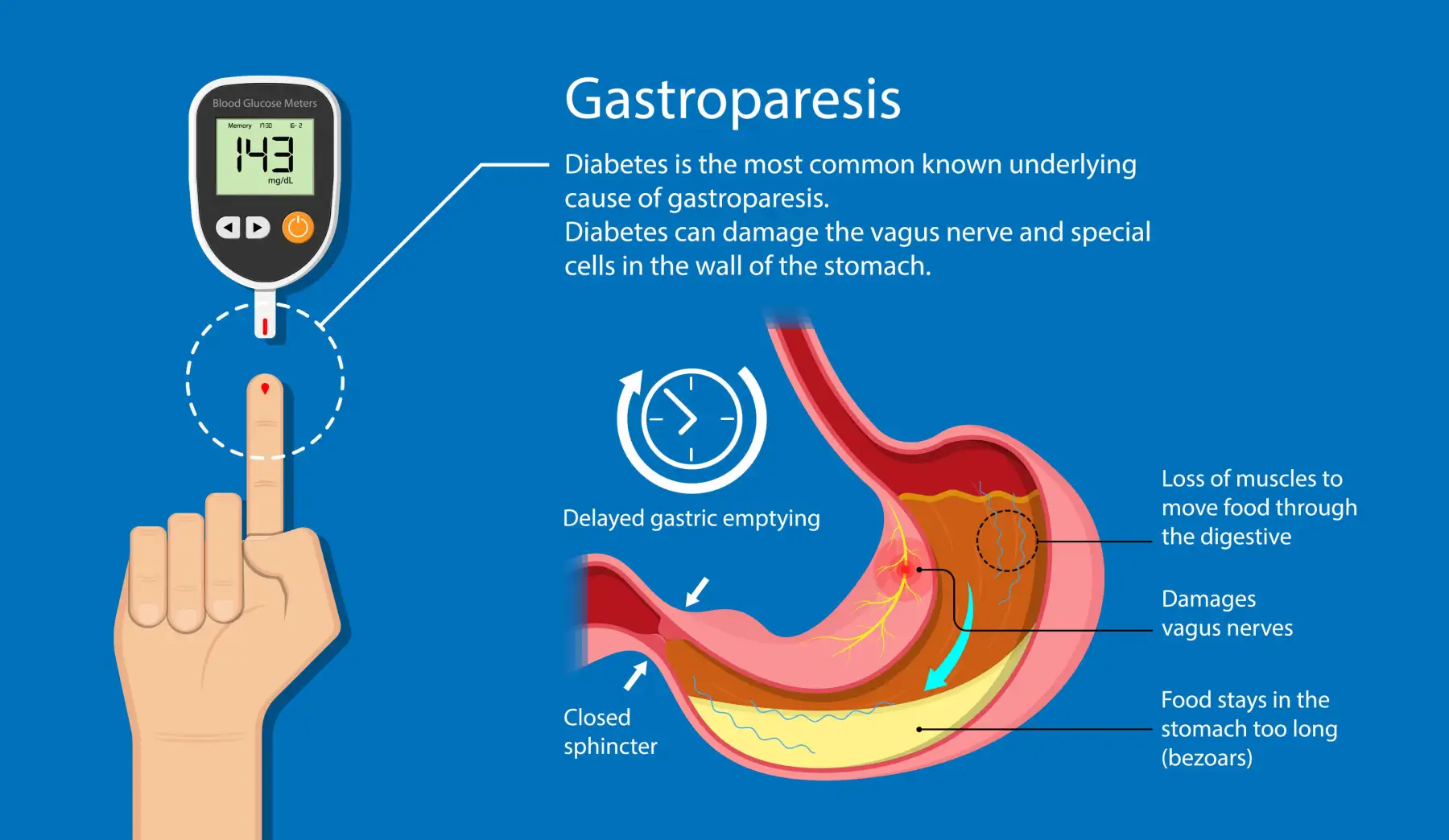
Bloedsuiker 3- Diabetiese Gastroparese Hoënormale Bloedsuiker en diabetes veroorsaak op ‘n stadige onbewustelike wyse dat persone se spysvertering nie na wense is nie. Die toestand kan as “slow poison” beskou word omdat hoënormale bloedsuiker en diabetes die senustelsel wat betrokke is by spysvertering, met tyd verswak en uiteindelik kan vernietig. Die toestand staan bekend as …
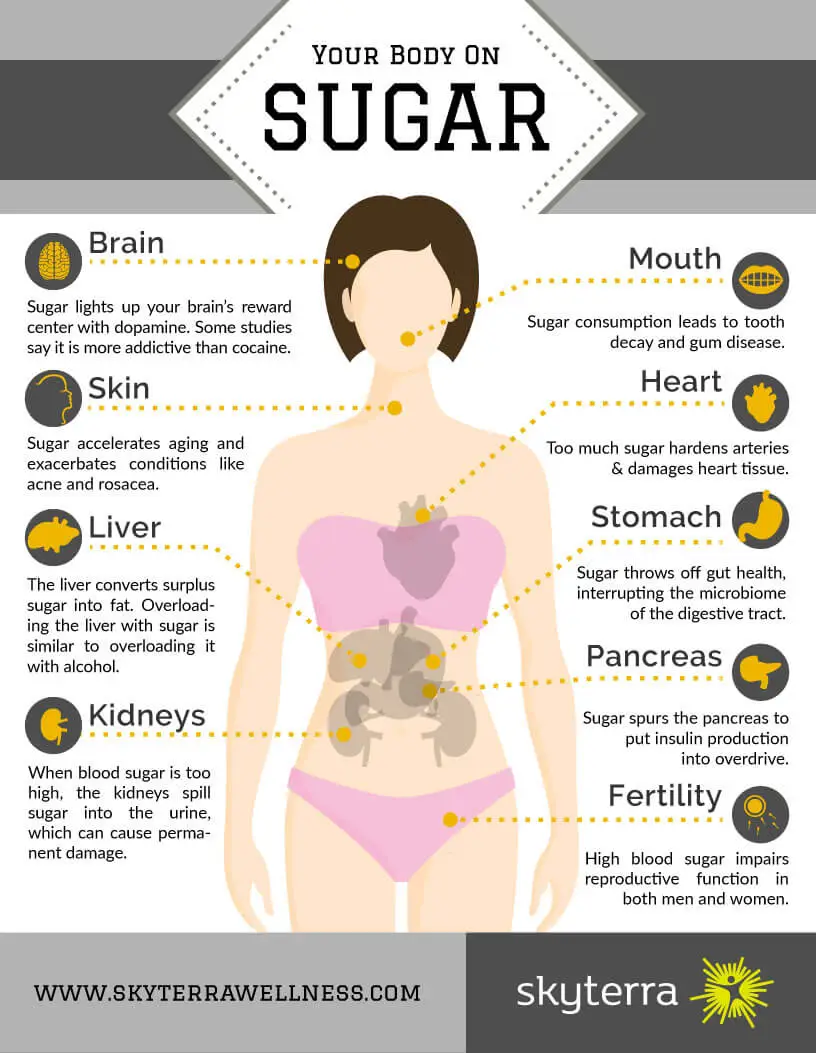
Die balansering van elke persoon se bloedsuiker is van uiterste belang. Bloedsuiker uit balans laat die hele liggaam daaronder lei en saal verwoesting onder al die selle van die liggaaam.
Blood sugar and the autonomic nervous system—the part of the nervous system that “automatically” regulates our internal organs while we go about our lives —controls the movement of food through the digestive tract. Blood sugar controls the vagus nerve, which controls the muscles of the stomach, tells the muscles to contract after a meal or snack to break up food and move it along to the small intestine. But if the vagus nerve is damaged, by high levels of blood sugar, the muscles of the stomach don’t work normally, and the movement of food slows or even grinds to a halt.
What is PCOS?
PCOS is a set of symptoms related to a hormonal imbalance that can affect women and girls of reproductive age. Women with PCOS usually have at least two of the following three conditions:
1. Absence of ovulation, leading to irregular menstrual periods or no periods at all.
2. High levels of androgens (a type of hormone) or signs of high androgens, such as having excess body or facial hair.
3. Cysts (fluid-filled sacs) on one or both ovaries—”polycystic” literally means “having many cysts.”




Recent Comments